In making decisions about medical care everyone should factor in cost—patients, doctors health insurance companies and government. Consider two alternative procedures, A and B. If for each $1,000 spent on procedure A, patients gain one extra month of life whereas using procedure B costs $2,000 for the same gain, A should be preferred to B. By making the efficient choice we free up money to meet other health and non-health needs.
There remains this problem, however: what if the person who makes the decision about cost is different from the person who realizes the gain. That is what gives rise to charges of “rationing” and “death panels.”
Aaron Carrol writes:
Other countries routinely use cost-effectiveness data to make decisions about health coverage. In Britain, the National Institute for Health and Care Excellence, a government agency that gives guidance about which services the National Health Service should cover, has a threshold of 20,000 to 30,000 pounds per QALY (about $31,000 to $47,000). They don’t make decisions on whether to cover therapies based on this number alone, but it is certainly considered a factor.
Where a QALY is a quality-adjusted year of life. And since government health care budgets are strained everywhere in the world, you can be sure that the cost effectiveness criteria is “considered” a lot.
According to a 2002 World Health Organization report, 25,000 cancer patients die prematurely in Britain each year—often because of lack of access to drugs generally available in the United States and Europe. (See also this 2013 NHS estimate on all causes of premature deaths.)
To use an example closer to home, in 1994 Hillary Clinton decided that as part of her own health reform, health plans would provide free mammograms only to women 50 and older—and only at two-year intervals. In contrast, the National Cancer Institute and the American Cancer Society at the time were recommending mammograms for women after 40, either annually or every other year, and yearly mammograms after 50. Similarly she hinted that she would relax the usual recommendation of a Pap smear every year for sexually active young women. (Canada, at the time, offered the test every three years.)
While these decisions were being made, a review of the literature by Tammy Tengs and her colleagues showed that:
- Annual mammograms for women age 55 to 64 were expected to cost $110,000 for every year of life saved.
- Annual mammograms for women in their 40s were expected to cost $190,000 per year of life saved.
In essence, Clinton decided that the lower number was an acceptable use of money while the higher figure was not. The review of the literature on Pap smears showed that:
- Screening young women for cervical cancer every four years costs less than $12,000 for every year of life saved—a very good deal in the risk avoidance business.
- More frequent screening causes the cost to soar from about $220,000 per year of life saved at three year intervals (as opposed to four year intervals) to $310,000 at two year intervals (as opposed to three).
- Giving Pap smears every year (as opposed to every other year) is really expensive: $1.5 million per year of life saved.
Clearly, Clinton and her advisors thought $1.5 million was way too high.
These decisions are said to have turned the general public against Hillary Care and doomed the Clinton health reform effort. But we shouldn’t take the wrong lesson away from that experience.
Hillary Clinton was not wrong about the cut off choices she made. She was wrong in thinking that the White House should make this decision for all the women of America. The tests involved are relatively inexpensive. They can easily be paid for from a Health Savings Account. If not getting a test is keeping someone awake at night, then by all means she should be encouraged to spend the money and get the test.
Here are some public policy principles to guide us going forward:
- Wherever possible, people should make their own decisions about risk—using money from savings accounts they own and control.
- Doctors should be encouraged to help patients make sensible decisions, based on their own knowledge of the literature on cost effectiveness. That is, doctors should be financial advisors as well as health advisors when their patients have to make choices about medical procedures.
- Insurance companies should be encouraged (and maybe even required) to reveal what standards they use in making coverage decisions and we should encourage an insurance market in which people can pay higher premiums for more generous coverage—especially if they are unusually risk averse.
- Government health programs should make coverage decisions that are in line with private sector insurance. And like private insurance, the government should announce a monetary cut off standard it is using. But we should encourage a secondary market for “top up” insurance—for example, providing coverage for expensive cancer drugs the government refuses to cover.
In case you missed it, Chris Conover has applied cost effective analysis to the entire Obamacare program, based on results from Massachusetts. He writes:
“.... even under the most wildly optimistic assumptions possible, Obamacare costs a jaw-dropping $224,000 per QALY. In the worst case, the costs would be as high as $1.3 million per QALY.”
He presents this chart (green = low estimate; red = high estimate):
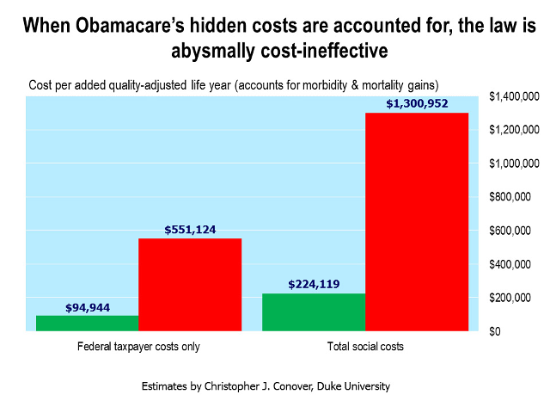
Photo credit: Christopher Conover, Duke University











